The word periodontal literally means “around the tooth.” Periodontal disease is a chronic bacterial infection that affects the gums and bone supporting the teeth. Periodontal disease can affect one tooth or many teeth. It begins when the bacteria in plaque (the sticky, colorless film that constantly forms on your teeth) causes the gums to become inflamed.
Periodontal (gum) diseases, including gingivitis and periodontitis, are serious infections that, left untreated, can lead to tooth loss.
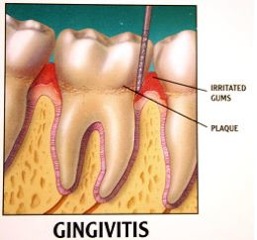
Gingivitis
Gingivitis, the first stage and the mildest form of periodontal disease, starts when the bacteria in dental plaque irritate the gums and cause infection. The bacteria in dental plaque irritate the gums and cause infection. When your body launches an immune response against these invaders, the gums become inflamed. People with gingivitis usually experience little or no discomfort. Therefore, it is important to recognize the symptoms, such as gums that are red, swollen or bleed easily. Gingivitis is reversible with professional treatment and good home oral care. Left untreated, gingivitis can lead to periodontitis.
Contributing Risk Factors:
- Diabetes
- Smoking
- Genetic predisposition
- Systemic diseases and conditions
- Stress
- Inadequate nutrition
- Hormonal fluctuations
- Pregnancy
- Substance abuse
- HIV infection
- Certain medications
Periodontitis
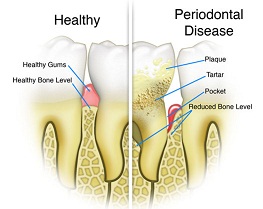 With time, plaque from untreated gingivitis can spread and grow below the gum line. Toxins produced by the bacteria in plaque irritate the gums. The toxins stimulate a chronic inflammatory response in which the body in essence turns on itself, and the tissues and bone that support the teeth are broken down and destroyed. Gums separate from the teeth, forming pockets (spaces between the teeth and gums) that become infected. As the disease progresses, the pockets deepen and more gum tissue and bone are destroyed. Often, this destructive process has very mild symptoms. Eventually, teeth can become loose and may have to be removed.
With time, plaque from untreated gingivitis can spread and grow below the gum line. Toxins produced by the bacteria in plaque irritate the gums. The toxins stimulate a chronic inflammatory response in which the body in essence turns on itself, and the tissues and bone that support the teeth are broken down and destroyed. Gums separate from the teeth, forming pockets (spaces between the teeth and gums) that become infected. As the disease progresses, the pockets deepen and more gum tissue and bone are destroyed. Often, this destructive process has very mild symptoms. Eventually, teeth can become loose and may have to be removed.
The most common forms of periodontitis include the following.
Aggressive periodontitis occurs in patients who are otherwise clinically healthy. Common features include rapid attachment loss and bone destruction and familial aggregation.
Chronic periodontitis results in inflammation within the supporting tissues of the teeth, progressive attachment and bone loss. This is the most frequently occurring form of periodontitis and is characterized by pocket formation and/or recession of the gingiva. It is prevalent in adults, but can occur at any age. Progression of attachment loss usually occurs slowly, but periods of rapid progression can occur.
Periodontitis as a manifestation of systemic diseases often begins at a young age. Systemic conditions such as heart disease, respiratory disease, and diabetes are associated with this form of periodontitis.
Necrotizing periodontal disease is an infection characterized by necrosis of gingival tissues, periodontal ligament and alveolar bone. These lesions are most commonly observed in individuals with systemic conditions such as HIV infection, malnutrition and immunosuppression.
Treatment
Periodontal health should be achieved in the least invasive and most cost-effective manner. This is often accomplished through non-surgical periodontal treatment, including scaling and root planing (a careful cleaning of the root surfaces to remove plaque and calculus [tartar] from deep periodontal pockets and to smooth the tooth root to remove bacterial toxins), followed by adjunctive therapy such as local delivery antimicrobials and host modulation, as needed on a case-by-case basis.
Usually after scaling and root planing, many patients do not require any further active treatment, including surgical therapy. However, patients will require ongoing maintenance therapy to sustain health. Non-surgical therapy does have its limitations, however, and when it does not achieve periodontal health, surgery may be indicated to restore periodontal anatomy damaged by periodontal diseases and to facilitate oral hygiene practices.
FAQs
Q: Is tooth loss a normal part of aging?
A: With good oral hygiene and regular professional care, your teeth are meant to last a lifetime. However, if left untreated, periodontal (gum) disease can lead to tooth loss. It is the primary cause of tooth loss in adults 35 and over.
Q: Does gum disease mean I have a “dirty mouth”?
A: Research proves that up to 30% of the population may be genetically susceptible to gum disease. Despite aggressive oral care habits, these people may be six times more likely to develop periodontal disease.
Q: Does gum disease affect overall health?
A: Emerging research links periodontal disease to other health problems including heart and respiratory diseases; preterm, low birthweight babies; stroke; osteoporosis; and diabetes.
Q: Is gum disease a mild infection?
A: The mass of tissue in the oral cavity is equivalent to the skin on your arm that extends from the wrist to the elbow. If this area was red, swollen, and infected, you would visit the doctor. Gum disease is not a small infection. Its result, tooth loss, leads to a very different lifestyle including changes in your appearance, breath, and ability to chew food.
Q: Are bleeding gums normal?
A: Bleeding gums are one of the warning signs of gum disease. Think of gum tissue as the skin on your hand. If your hands bled every time you washed them, you would know something is wrong. Other signs of gum disease include: red, swollen or tender gums; sores in your mouth; gums that have pulled away from the teeth; persistent bad breath; pus between the teeth and gums (leaving bad breath); loose or separating teeth; a change in the way the teeth fit together; and a change in the fit of partial dentures.
Q: Why can’t I just take oral antibiotics to treat my gum disease?
A: Periodontal bacteria live on the root surfaces of the teeth. Deep below the gumline, these bacteria develop a protective biofilm resistant to systemic antibiotics. The medicine is simply unable to reach the bacteria.
Q: What is Arestin?
A: ARESTIN® is a prescription antibiotic approved by the Food and Drug Administration (FDA). It is used together with scaling and root planing (SRP) procedures performed by a trained dental professional for the treatment of periodontal (gum) disease.
Q: Is the treatment for gum disease painful?
A: New periodontal procedures including local anesthesia and over-the-counter medications, have made patients’ treatment experiences pleasant and comfortable. Many patients find they are back to normal routines on the same day or by the next day.
Q: Why can’t I just have my regular cleaning?
A: The prophylaxis, or your “regular cleaning” is done to prevent disease. It is for “healthy” gums only. Once you have the disease, more aggressive treatment is now needed in order to get it under control.
Q: What is scaling and root planing (SRP)?
A: For periodontal (gum) disease treatment, dental professionals use a common mechanical procedure known as SRP. Scaling removes plaque, tartar and stains from the surface of teeth and their roots. Planing smoothes the rough areas on the roots of teeth to promote healing.
Q: Is it true that once teeth are lost, the only treatment options are crowns, bridges or dentures?
A: Dental implants are a permanent tooth-replacement option for teeth lost to trauma, injury or periodontal disease. Dental implants feel and look so natural that many patients forget they ever lost a tooth.
Q: Should pregnant women skip professional dental checkups?
A: Teeth and gums are affected during pregnancy like other tissues in the body. In order to decrease the risk of damaging the gums and tissues surrounding the teeth, pregnant women should schedule an appointment for a periodontal evaluation.